Randomization in Medical Device Clinical Trials: Everything You Need to Know
.png?width=800&height=400&name=Randomization%20in%20Medical%20Device%20Clinical%20Trials%20Everything%20You%20Need%20to%20Know%20(new).png)
The purpose of MedTech clinical investigations is to gain insights about the safety and effectiveness of a medical device. To ensure the quality of those insights, clinical trial sponsors and investigators employ various methods of experimental controls whose goal is to reduce the potential impact of bias on their experimental results.
In this blog, we’re focusing on a specific kind of experimental control that counteracts selection bias in medical device clinical studies: randomization. You’ll find answers to:
- What is randomization in clinical trials?
- What are the benefits of randomization in clinical trials?
- How does randomization work in clinical trials?
- What are the 3 types of clinical trial randomization?
- How can Greenlight Guru Clinical’s EDC software help with randomization in clinical trials?
What is randomization in clinical trials?
Randomized Controlled Trials (RCTs) have become the gold standard for MedTech clinical investigations, as they provide the most reliable and unbiased evidence about the safety and effectiveness of medical devices.
In an RCT, clinical investigators allocate study participants into two or more groups that will receive different interventions as part of the study. Some participants may be assigned to a “control group” where they receive the existing standard of care, while others may be assigned to a “treatment group” where they receive an experimental treatment involving the novel medical device. Some clinical studies involve more than one treatment group, allowing investigators to test different protocols for the experimental treatment.
Randomization is a method of assigning participants in a medical device study to treatment and control groups while ensuring that each participant has an equal and unbiased chance of being assigned to any group.
The purpose of randomization in medical device clinical trials is to protect the reliability of experimental results by eliminating the selection bias that can naturally manifest when study participants are manually assigned to treatment or control groups by researchers.
What are allocation concealment and blinding in clinical trials?
Allocation Concealment and Blinding are two additional types of experimental controls, often used in conjunction with randomization to counteract bias in clinical investigations.
Randomization in clinical trials is sometimes implemented via the creation of a randomly generated allocation sequence. Once generated, the random allocation sequence can be applied to a list of study participants, randomly assigning each participant to a control or treatment group based on their position in the list.
Allocation Concealment is a technique where the random allocation sequence is kept hidden from researchers assigning participants to treatment groups until the moment of assignment. This technique prevents researchers from modifying the participant list or changing how the sequence is applied to influence which participants are assigned to which intervention groups.
Allocation concealment is sometimes confused with blinding, but they aren’t quite the same thing.
Blinding is a type of experimental control where information is hidden from the participants in a clinical investigation to avoid biasing the results of the study. The two most common implementations of blinding in RCTs are:
- Single-blind studies, where the study participant does not know to which intervention group they are assigned (e.g. control group, placebo group, experimental group, etc.).
- Double-blind studies, where neither the participants nor the investigators measuring treatment outcomes and completing eCRF forms know to which intervention group each study participant was assigned.
Double-blind studies provide two important benefits when it comes to reducing bias: patients are not influenced by knowing whether they received the control or the experimental treatment, and researchers cannot treat patients or interpret their clinical outcomes differently based on prior knowledge of which treatment they received.
Clinical trial sponsors using electronic data capture (EDC) software like Greenlight Guru Clinical can customize collaborator permissions, exercising full control over who can generate, view, or export randomized allocation lists for clinical investigations.
How does randomization work in clinical trials?
Randomization in clinical trials is applied from the outset, when study participants are being assigned to their respective intervention groups. Randomization involves the creation of a randomly generated allocation sequence that will be applied to a list of participants, assigning each one to a random intervention group.
The randomization process can be implemented by researchers in multiple ways with varying levels of complexity. Randomization can be done manually, but leading researchers today use software tools like Greenlight Guru Clinical’s randomization module to automate the randomization process and eliminate any potential for selection bias.
Below, we explain three types of clinical trial randomization and how they work.
3 types of randomization you should know
1. Simple Randomization
Simple randomization is when patients are assigned to intervention groups based on a single sequence of random assignments.
Simple randomization is the least complex randomization method: researchers go through a list of study participants and assign each one to a treatment group using an arbitrary random method such as a coin flip (heads for control, tails for experimental), a shuffled deck of cards (red for control, black for experimental), or rolling a die (even numbers for control, odd numbers for experimental)
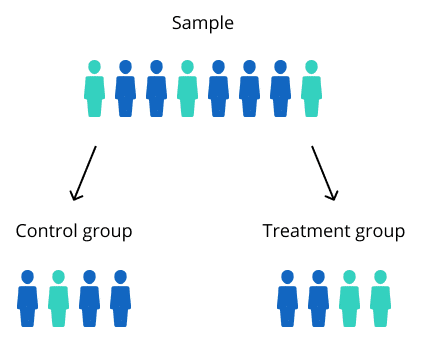
Simple randomization uses arbitrary random methods to assign participants to either a control or a treatment group
(Source)
Simple randomization can work well for larger studies, but may result in an unequal number of participants across intervention groups when implemented in studies with a small sample size. Simple randomization also fails to control for any kind of systematic variance between groups that could impact experimental results.
2. Block Randomization
Block randomization is an improvement on simple randomization that ensures an equal number of participants will be allocated to each intervention group.
In block randomization, study participants are grouped into “blocks” of a predetermined size. The size of each block depends on the number of intervention groups that are planned for the study. Once the blocks have been formed, researchers use randomization to determine how the patients in each block will be allocated to the various treatment groups.
A study with just two intervention groups (control and experimental) and 100 participants might divide those participants into twenty-five blocks with 4 people in each. Given a block size of 4, there are six possible ways (permutations) to equally divide the participants in each block equally between the two treatment groups. The researchers would then use a random method to choose one of these permutations and use it to equally assign each block’s participants to a random treatment group.
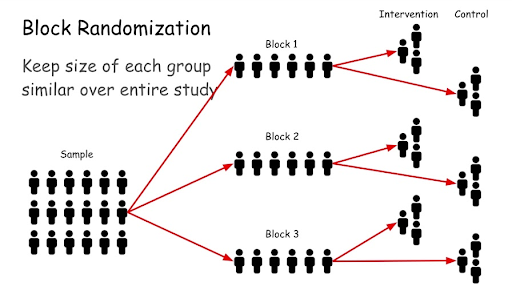 Block Randomization allocates participants randomly into treatment groups while ensuring that all treatment groups remain similar in size. (Source)
Block Randomization allocates participants randomly into treatment groups while ensuring that all treatment groups remain similar in size. (Source)
Block randomization ensures that participants are allocated equally and randomly between treatment groups, but it does not necessarily result in groups that are statistically balanced for external variables (e.g. age, sex, concomitant medications, prevalence of secondary diseases, etc.).
3. Stratified Randomization
Stratified randomization can be used to ensure that treatment groups are balanced for external variables like age, gender, prevalence of secondary diseases, etc. that could impact clinical outcomes.
In stratified randomization, researchers collect covariate data from subject participants and intentionally group participants with similar baseline characteristics (e.g. age, sex, secondary diseases, medical history, etc.) into the same blocks. From here, block randomization is applied to equally and randomly assign the participants in each block to an experimental group.
By allocating participants with similar characteristics equally across all intervention groups, researchers can minimize the impact of external variables and increase the reliability of their experimental results.
What are the benefits of randomization in clinical trials?
In this section, we are listing 3 clear benefits we have identified for using randomization in medical device clinical studies.
1. Randomization Reduces or Eliminates Selection Bias
The alternative to randomization is allowing clinical investigators to manually assign study participants to intervention groups. This is not desirable because it introduces selection bias - the bias that exists when individuals make subjective choices - into the study.
Selection bias in the intervention group allocation process happens when researchers allow their allocation decisions to be influenced by prior beliefs or other external factors. Examples of selection bias in group allocation could include things like:
- A researcher allocates the most unwell/symptomatic subjects to the experimental group because they believe the experimental medical device will help them.
- A researcher allocates the least unwell/symptomatic subjects to the experimental group because they believe the experimental medical device will not be effective.
- A researcher allocates elderly subjects to the control group because they believe the experimental treatment might be painful or unpleasant for them.
- A researcher wants the study to succeed, so they allocate subjects whose conditions are most likely to improve into the experimental group.
- A researcher wants the study to fail, so they allocate the most difficult cases (least likely to have good clinical outcomes) into the experimental treatment group.
As you can see, there are many ways in which a researcher's beliefs about the study could influence how they would choose to allocate participants. Allowing researchers to manually allocate subjects into intervention groups has the potential to significantly bias results. One study found that trials with inadequate randomization tended to overestimate treatment effects by up to 40% compared to studies that used proper randomization.
2. Randomization helps control for systematic variance
In addition to controlling for selection bias, randomization techniques can help ensure that participants in the various treatment groups of a clinical investigation do not vary in a systematic way.
Consider a medical device clinical investigation with 100 participants allocated equally between a control group and an experimental treatment group. If the participants in the control group have a significantly higher age, average BMI, or a higher rate of disease compared to the experimental treatment group, an imbalance has been created that could affect the results of the trial.
Randomization techniques help clinical researchers construct groups that are as similar as possible to avoid the obfuscating impact of confounding variables and ensure the reliability of their results.
3. Randomization forms the basis for statistical testing
At the conclusion of a clinical investigation, researchers want to compare clinical outcomes between intervention groups using statistical testing to either accept or reject the null hypothesis.
But if the allocation of study participants between intervention groups is non-random, or if the participants in different groups vary in a systematic way outside of which treatment they received, researchers can no longer rely on statistical testing to indicate whether the novel medical device was truly more effective than the current standard of care.
Because of this, it can be said that proper randomization in clinical investigations forms the basis for reliable statistical testing that determines whether the experimental medical device produced a measurable improvement in patient care outcomes.
Randomize your clinical investigations with
Greenlight Guru Clinical
Greenlight Guru Clinical's Randomization module is the medical device manufacturers' top module choice for its easy setup and study results reliability.
The module supports block randomization with variable block sizes as well as stratified randomization, giving clinical investigators the maximum flexibility to create high-quality, statistically balanced and unbiased intervention groups for clinical investigations.
Schedule an intro call and see how you can maximize your clinical investigation efficiency with Greenlight Guru Clinical's electronic data capture capabilities.
Jón Ingi Bergsteinsson, M.Sc. in Biomedical Engineering, is the co-founder of Greenlight Guru Clinical (formerly SMART-TRIAL). He was also the technical founder of Greenlight Guru Clinical where he paved the way for the platform’s quality standards, data security, and compliance.

.png?width=790&name=15-in-1%20clinical%20investigations%20content%20bundle%20(new).png)



